Posts Tagged ‘fungus’
Common Nail Fungus Symptoms and Solutions
Common Nail Fungus Symptoms and Solutions
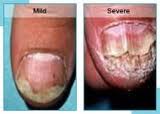 Suffering from some form of nail fungus is very common in humans. Because we find this embarrassing, we tend to hide the infected nail from view. This is especially true with toenails as they are easiest to hide inside a stuffy, warm set of shoes and socks.
Suffering from some form of nail fungus is very common in humans. Because we find this embarrassing, we tend to hide the infected nail from view. This is especially true with toenails as they are easiest to hide inside a stuffy, warm set of shoes and socks.
Solving this problem can be both easier, and more difficult than you think. There are many products available to cure nail fungus. However some of them include some risk of further problems, some don’t and will never work, and some people just have the problem of poor health that leads to continued infection.
What Causes Nail Fungus?
Every day we encounter many different microbes, microorganisms and bacterial. This is a normal part of life. Some of these turn out to be nail fungus spores. Most of the time, these are harmless as they are easily washed away. But if they manage to get into or under your nails, then they become problematic.
When the spore gets itself into a warm, dark, moist place on your body (most commonly your nails because they have that extra benefit of being a good shield from the world) they are able to grow and multiply, causing that nasty look of yellowing and thickness everyone associates with a nail fungus infection.
As the invasion by the fungus develops, so do the symptoms of nail fungus infection. The nail begins to become disfigured and can even get to the point where it crumbles or flakes away. This is most common in toenails because they spend so much time wrapped in socks and shoes, which creates a great breeding environment for the fungus.
How Do I Treat a Nail Fungus Infection?
There are several natural remedies available, as well as many home remedies that are recommended before you try the more aggressive method of taking an oral antifungal medication, which carries the risk of damage to your liver. Here are some suggestions:
• Tea Tree Oil – This natural essential oil is available at most health food stores. Rub the oil into the nail and surrounding skin a few times a day. Its antifungal properties will eventually kill the fungus
• Good Nail Hygiene – Keep your nails short, right at the edge of the toe and clean out the underside with a nail file to ensure no dirt is able to permanently lodge there. Keep your feet clean and dry and air them as much as possible by not wearing closed shoes.
• Vinegar – Soak your toes in a solution of vinegar and water, then wash and dry them thoroughly. The vinegar changes the pH of the growing environment, making it uninhabitable for the fungus.
If you have tried these solutions, and/or some of the others out there and nothing seems to make the nail fungus infection go away permanently, your next step is to consult with your health care professional to find a more standard medical solution to the problem. Be aware that some of these prescription solutions do carry risks so be sure to discuss this with your doctor and to make your doctor aware of all medications your are currently taking. During your treatment, continue to practice good nail hygiene as this will encourage the healing process and help to prevent spreading or continued nail fungus infection of your toenails.
Many solutions are available to treat this problem. Search the internet for alternatives before you commit yourself to taking an oral antifungal medication, especially if a child is the infected patient. If you do your research it will pay off in the long run.
A Doctor’s Detailed Description of Onychomycosis
A Doctor’s Detailed Description of Onychomycosis
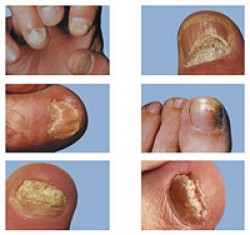 Onychomycosis is the medical term for a fungal infection of the fingernails or toenails. Onycho refers to the nail, mycosis refers to fungal infection. This condition represents about 33% of all fungal skin infections. Approximately half of all diagnosed diseases of the fingernails or toenails are onychomycosis.
Onychomycosis is the medical term for a fungal infection of the fingernails or toenails. Onycho refers to the nail, mycosis refers to fungal infection. This condition represents about 33% of all fungal skin infections. Approximately half of all diagnosed diseases of the fingernails or toenails are onychomycosis.
Onychomycosis usually occurs in older people, most commonly 40 and above. The likelihood of the disease occurring in adults rather than children is about 30%. Onychomycosis is a regularly occurring disease and the chances of contracting it increase as people age. Approximately 20% of all people between the ages of 40 and 60 have onychomycosis. It is thought that upwards of 90% of elderly patients have it.
Onychomycosis occurances
Onychomycosis occurs more regularly in men than in women, however women are more likely to contract a specific type of the fungus called Candida. The disease seems to have no preference in race. There has been an increase in the number of cases of onychomycosis in recent years. Doctors believe this has to do with people living longer, thus facing the greater probability of diseases that are common causes of onychomycosis. For instance, the level of diabetes has increased in the population as well. The same corollary can be drawn between the aging population and the number of people with diabetes. Interestingly enough, having diabetes makes it more likely that a patient will contract onychomycosis as diabetics have a harder time fighting off infection and healing from wounds. Poor circulation is another commonly related disease as people who suffer from this have a less healthy immune system.
The most common symptom and complaint of sufferers of onychomycosis is the disfiguration of the nail. One of the greatest difficulties in catching a fungal nail infection early on is that it doesn’t present serious symptoms, especially in the beginning, when it is easiest to cure.
The fact that onychomycosis disfigures the nail is not to be disregarded. It causes people to avoid certain social interactions because of the embarrassment they feel having a nail fungus will bring. They become concerned that a fungal infection is infectious or that they will be seen as “unclean” or “unhealthy”. It is of serious concern to doctors, the psychological and emotional effect that onychomycosis can have on people.
Although this disease starts as a series of cosmetic symptoms, if left unchecked it can develop into a far more serious set of problems. Pain in the affected finger or toe can occur. Because the nail thickens, it deadens the sensitivity in the affected digits. This can lead to loss of sensation and therefore ability in the hands and feet. Tasks like writing and other daily activities are affected by fingernail fungus, being able to sense the floor, causing difficulty with walking and even causing serious falls, are an advanced symptom of toenail fungus. For patients who are already affected by diseases that cause problems with the nerves in the legs, this can make things even worse.
There are four main types of onychomycosis:
- Distal subungual onychomycosis – This is the most common form of onychomycosis and is caused by a dermatophyte called Trichophyton rubrum. What happens is the dermatophyte penetrates the nail plate and buries itself in the nail bed. The term ‘subungual’ refers to underneath the nail. The infection manifests as a whitish-yellow growth under and on the nail towards the tip (the part you trim) This then works its way down toward the cuticule and underneath to the nail bed. The nail becomes thick, pitted, ridged and can start to crumble.
- Proximal subungual onychomycosis – starts at the cuticle end of the nail instead of at the tip. It then works its way up the nail and under the nail as the nail grows out. This form of nail fungus infection occurs more regularly in people who have issues with immune deficiency. Proximal subungual onychomycosis is caused by Trichophyton ruburm, just as distal subungual onychomycosis is, but it is also caused by other fungi and molds.
- White superficial onychomycosis – This is probably the least commonly occurring form of onychomycosis, happening in only 1 of 10 cases on average. This fungus develops on the top of the nail or in its topmost layers. As the name ‘white superficial’ would imply, this is a lesion that forms at the top of the nail and is white in color. Gradually, the fungus will take over the entire nail if left unchecked. Unlike most other forms of onychomycosis, white superficial onychomycosis is caused by Trichophyton mentagrophytes, a different dermatophyte.
- Candida onychomycosis – This final form of onychomycosis starts out its life as chronic mucocutaneous candidas, or reoccurring mucous level or low level yeast infection. This tends to affect the skin surrounding the nail, specifically in the proximal and lateral nail folds. Usually multiple nails are affected by Candida onychomycosis and the nails can be fully destroyed by this more serious form of fungal infection.
References
Hainer BL. Dermatophyte infections. Am Fam Physician 2003;67:101-108.
Jaffe R. Onychomycosis: recognition, diagnosis, and management. Arch Fam Med 1998;7:587-592.
Kaur R, Kashyap B, Bhalla P. Onychomycosis–epidemiology, diagnosis and management. Indian J Med Microbiol 2008;26:108-116.
Paronychia
Paronychia
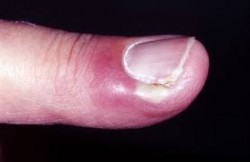 aronychia is a disease of the Perineum, where the skin around the surface of the nail hangs loosely. It has been found most often in the U.S., usually in kids who have a habit of biting their nails or sucking their fingers. There two forms of Paronchial infection, Chronic Paronychia and Acute Paronychia. The forms are judged according to the length of time it remains in the body.
aronychia is a disease of the Perineum, where the skin around the surface of the nail hangs loosely. It has been found most often in the U.S., usually in kids who have a habit of biting their nails or sucking their fingers. There two forms of Paronchial infection, Chronic Paronychia and Acute Paronychia. The forms are judged according to the length of time it remains in the body.
Paronychia is a viral infection that grows gradually stronger, resulting in a bumpiness, softness and redness surrounding the nails. The main culprits for this infection are Candida and mold. It can be passed from person to person via touch.
Causes of Paronychia
Most forms of Paronychia occur by a nick or break in the skin being infected. If a person has a hangnail or a habit of chewing their nails, this is a good way for the infection to enter the area. There is evidence of Streptococcus and Pseudomonas germs getting into the infected area and making it worse. The chronic form of Paronychia is typically linked with the use of abrasives, for instance soaps and detergents while washing. The chronic infections are typically the result of Candida albcans or other fungus.
Acute Paronychia occurs when the skin around the nail becomes inflamed and swells causing pain to the afflicted person. Pus may develop and ooze from the infected area, removing the top layer of the nail.
Chronic Paronychia is a longer lasting case and the nails can become so infected that they develop a greenish tinge around the edges of the skin.
Diagnosis
In the cases of Acute Paronychia, a culture of the pus can be taken to determine what kind (or kinds) of infection is occurring and then treatment can be prescribed. Chronic Paronychia can be a bit more difficult to diagnose and treat, though a potassium hydroxide test may be able to determine which fungus is the source of the infection.
Treatment
- Massaging the afflicted area in hot water three to four times per day can help relieve some of the pain and swelling
- Antibiotics such as diclogacilin and cephelaxin may be prescribed
- If the swelling is severe, the area may need to be punctured and drained
- Part of the nail may need to be removed in some cases
- An antifungal may also be prescribed
Things that should NOT be used to cure Paronychia
- Do not use topical antibiotics
- Do not take prescribed steroids
Unusual cases of people who have contracted Paronychia have occurred in patients with:
- HIV/AIDS
- On steroids
- High blood sugar
- Poor circulation
Prevention
- Don’t chew or bite your nails
- Don’t suck on your fingers or thumbs
- Don’t immerse your hands in water without wearing protective gloves