Archive for the ‘Nail Fungus Symptoms’ Category
What are the symptoms of a Nail fungus and how can I tell if I have a Nail Fungus Infection?
What are the symptoms of a Nail fungus and
how can I tell if I have a Nail Fungus Infection?
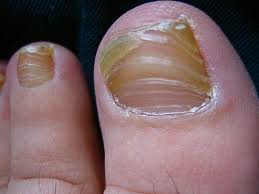 You’d think these would be fairly straightforward questions that ought to illicit simple answers. Unfortunately not only is this not true, but it is confusing enough that sometimes doctors misdiagnose nail fungus (or onychomycosis). Knowing the symptoms will assist you in helping your doctor to order the appropriate diagnostic tests so that you end up with the correct solution to your problem.
You’d think these would be fairly straightforward questions that ought to illicit simple answers. Unfortunately not only is this not true, but it is confusing enough that sometimes doctors misdiagnose nail fungus (or onychomycosis). Knowing the symptoms will assist you in helping your doctor to order the appropriate diagnostic tests so that you end up with the correct solution to your problem.
There are two basic causes of nail infections. Bacterial and fungal. Onychomiycosis, or fungal nail infection, is usually caused by a dermatophyte called Trichophyton rubrum. If not, it is caused by Candida albicans, a yeast growth (also a fungus). As nail infections differ in variety and in cause, the correct cure must be applied. A fungal infection should be treated with an anti-fungal whereas a bacterial infection should be treated with an antibiotic.
Onychomycosis affects the nail bed (skin underneath the nail) nail plate (the hard surface that we refer to as the nail) or the skin around the nail. About one third of skin infections and half of nail infections are caused by Onychomycosis. The visual signs are the abnormalities caused by the nail fungus. A white or yellowish crust appears on top of or embedded in the nail. This is the actual fungus growth. Sometimes it appears as streaks that follow the line of the nail against the infected digit (finger or toe) and sometimes it appears at the cuticle (soft area at the base of the nail). As the fungus spreads, it covers the entire surface of the nail, turning it to a milky white or yellow. Frequently it causes the nail to become ridged and deformed. This is a result of the dermaptophytes emitting destructive waste product as a result of consuming keratin. If the fungus gets underneath the nail plate, it can cause the nail bed to become irregular. This causes the nail plate to release from the bumpy nail bed and the nail becomes loose and can fall off.
If the nail fungus infection becomes severe, or if it contains Candida, the area around the nail can become swollen and sensitive to the touch. The skin may express (think ooze) pus and be very uncomfortable, even painful. These are common signs of infection. The pus is a result of white blood cells rushing to the area to fight off the infection. This is your body trying to do its job and tell you and your doctor that something is wrong.
It is most common for pus to be present in the case of bacterial infections. Thus your doctor should check for this before looking for fungal infections. To add to the confusion, there are diseases that mimic a nail fungus, including hallopeau acrodermatitis, lichen planus, nail bed psoriasis (which can occur in conjunction with fungal infection of the nail), nail bed melanoma, Reiter syndrome, yellow nail syndrome, onycholysis, and paronychia. Because of this factor, more than one test may be necessary to determine the correct course of treatment.
Different forms of onychomycosis will require different samples from the affected area. In some cases the nail can be sampled from the end or the top can be scraped for a sample, in others, the nail will need to be removed entirely. Whereas this can be a bit scary, it is also to your advantage as it then exposes the nail bed so that it can be treated.
The most typical tests performed on a nail culture to look for onychomycosis are a potassium hydroxide wash, which allows for the sample to be put under a microscope and searched for evidence of fungal growth, or a fungal culture, where the sample piece of nail is put in an environment (usually a petri dish) where it has the necessary components to thrive and create new growth, thus showing what kind of fungal infection it is. In the unlikely event that neither of these tests show positive for onychomycosis, the remaining nail sample can be pulverized and sent to a pathology lab for analysis or submitted for a bacterial culture if it is determined that the infection is bacterial instead of fungal.
Determining what kind of infection you have and what to do about it are very important when dealing with a nail infection of any kind. Having the infected area looked at by a physician, preferably a dermatologist, is the best way to deal with these diseases as they can help to rule out and diagnose serious problems as well as knowing what to do about the infection in the first place.
Koilonychia
Koilonychia
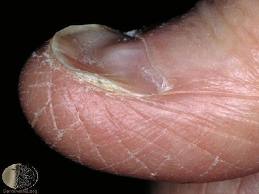 Koilonychia is a hereditary disorder that affects the fingernails. The nails start to get thinner and end up lifting at the outer edges, a condition more commonly known as spoon nails. This is caused by the poor absorption of iron into the bloodstream, also known as anemia.
Koilonychia is a hereditary disorder that affects the fingernails. The nails start to get thinner and end up lifting at the outer edges, a condition more commonly known as spoon nails. This is caused by the poor absorption of iron into the bloodstream, also known as anemia.
What Causes Koilonychia?
The following are common causes of Koilonychia:
- Poor circulation
- Poor Thyroid Function
- Muscle Skinning Condition
- Universal Lupus
- Hemochromatosis
- Patella Syndrome
- Reynaud’s Syndrome,
- Erythematosus
- Poor health
- Iron deficiency
- Overuse of soaps and oils
- Glossitis
- Cheilosis
- Pica
- Undernourishment
Symptoms and Solutions
Koilonychia is a symptom of anemia and/or iron deficiency. It needs to be caught quickly once the visual symptoms have shown. Granted, spoon nails can also be caused by worrying the edge of the nail, causing them to detach from the nail bed and curl up. However there are many ways that Koilonychia can be prevented.
- Wear protective covering on your hands while washing dishes or immersing your hands in liquid for a long period of time.
- Don’t bite your nails as this can cause irritation and inflammation to the nail bed
- Obtain proper nourishment whenever possible
- Take vitamin supplements
- Work with your doctor to identify the cause of your anemia and supplement your diet accordingly.
- Don’t eat or drink things that cause your system to shed iron, for instance, caffeinated beverages slow down iron absorption.
- Take vitamin C and Iron supplements to increase healthy nail growing capacity.
Treatment usually consists of taking an iron supplement once or twice a day, and/or increasing the iron rich foods in the affected patient’s diet. The intestinal system may or may not allow the full absorption of the increased iron dosage, depending on the person.
Easily Applied Home Nail Fungus Remedies
Easily Applied Home Nail Fungus Remedies
 Having unattractive toenails is embarrassing and even humiliating. There are many ways to solve this incredibly common problem.
Having unattractive toenails is embarrassing and even humiliating. There are many ways to solve this incredibly common problem.
How Does My Nail Become Infected?
Toenails come into contact with microorganisms that get onto the skin, the nail sheath and underneath the nail to the nail bed. Any and all of these places can easily become a hotbed (literally) for infection. Once you have contracted a fungal infection, it can be very difficult to cure.
As these microorganisms are fungal spores, they thrive in places that have no light and high humidity. This makes the feet very susceptible to infection because we are all accustomed to wearing shoes. Especially because many people wear the same pair of shoes day in and day out, not allowing time for them to dry and air between wearings.
Trimming your toenails too close to the skin can cause accidental cuts, providing another entry point for these fungal spores.
Shoes that fit to tightly can also be a cause of toenail fungus infection as they leave no room for your feet to breath and they can cause the breakdown of the nail where they rub, leaving an opening for the fungus to invade.
Standard Symptoms of Nail Fungus Infection
Here are some very simple ways to recognize a toenail fungus infection:
- A discoloration of the toenail, white to yellow
- The nail becomes thick and disfigured
- A stinging pain from under and around the nail
- Brown or black spots developing on the nail
- Parts of the nail crumble or flake off
- A foul odor coming from the nail
- Oozing pus from around the nail
- Toenail falling off entirely
Recommended Home Remedies for Fungal Nail Infection
The faster you catch a fungal nail infection, the easier it is to get rid of it. The early stages can be treated with any of the remedies listed below:
- ClearFungus – This is the leading natural remedy for curing toenail fungus. This is considered more of a natural product anti-fungal treatment than a home remedy as it is specially formulated to kill toenail fungus and promote new nail growth.
- Vicks VapoRub – Although no one quite understands why, Vicks VapoRub seems to prove very effective at stopping the growth of fungal infection. It does not kill the fungus but does inhibit growth, which can encourage healthy nail growth until the infection has been trimmed entirely away. No studies have been done on this but many people swear by it.
- Hydrogen Peroxide, Listerine and Rubbing Alcohol – Combined or separately, all of these chemicals have been shown to have some effect on nail fungus as they all posses antiseptic properties. Soak your toenails in your choice of these solutions (again, combined or separately) for twenty minutes, two times a day.
- Tea Tree Oil – This is a powerful essential oil that contains antiseptic and antifungal components. Wash and thoroughly dry the foot, then rub the affected nail(s) and surrounding skin with Tea Tree Oil twice a day.
- Vinegar – Soaking your toes in a solution of equal parts vinegar and water in a large tub or bowl for 20-30 minutes, then washing and thoroughly drying your feet until the infection has cleared.
These remedies are good for stopping the infection early on. If you follow these instructions closely and stick to the regular process, you should be able to clear up your infection by yourself. If your symptoms are bad to begin with, or if they worsen, seeking the help of a medical professional will become necessary.
A Doctor’s Detailed Description of Onychomycosis
A Doctor’s Detailed Description of Onychomycosis
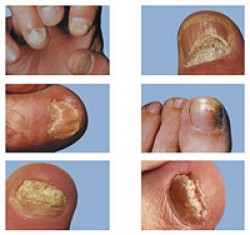 Onychomycosis is the medical term for a fungal infection of the fingernails or toenails. Onycho refers to the nail, mycosis refers to fungal infection. This condition represents about 33% of all fungal skin infections. Approximately half of all diagnosed diseases of the fingernails or toenails are onychomycosis.
Onychomycosis is the medical term for a fungal infection of the fingernails or toenails. Onycho refers to the nail, mycosis refers to fungal infection. This condition represents about 33% of all fungal skin infections. Approximately half of all diagnosed diseases of the fingernails or toenails are onychomycosis.
Onychomycosis usually occurs in older people, most commonly 40 and above. The likelihood of the disease occurring in adults rather than children is about 30%. Onychomycosis is a regularly occurring disease and the chances of contracting it increase as people age. Approximately 20% of all people between the ages of 40 and 60 have onychomycosis. It is thought that upwards of 90% of elderly patients have it.
Onychomycosis occurances
Onychomycosis occurs more regularly in men than in women, however women are more likely to contract a specific type of the fungus called Candida. The disease seems to have no preference in race. There has been an increase in the number of cases of onychomycosis in recent years. Doctors believe this has to do with people living longer, thus facing the greater probability of diseases that are common causes of onychomycosis. For instance, the level of diabetes has increased in the population as well. The same corollary can be drawn between the aging population and the number of people with diabetes. Interestingly enough, having diabetes makes it more likely that a patient will contract onychomycosis as diabetics have a harder time fighting off infection and healing from wounds. Poor circulation is another commonly related disease as people who suffer from this have a less healthy immune system.
The most common symptom and complaint of sufferers of onychomycosis is the disfiguration of the nail. One of the greatest difficulties in catching a fungal nail infection early on is that it doesn’t present serious symptoms, especially in the beginning, when it is easiest to cure.
The fact that onychomycosis disfigures the nail is not to be disregarded. It causes people to avoid certain social interactions because of the embarrassment they feel having a nail fungus will bring. They become concerned that a fungal infection is infectious or that they will be seen as “unclean” or “unhealthy”. It is of serious concern to doctors, the psychological and emotional effect that onychomycosis can have on people.
Although this disease starts as a series of cosmetic symptoms, if left unchecked it can develop into a far more serious set of problems. Pain in the affected finger or toe can occur. Because the nail thickens, it deadens the sensitivity in the affected digits. This can lead to loss of sensation and therefore ability in the hands and feet. Tasks like writing and other daily activities are affected by fingernail fungus, being able to sense the floor, causing difficulty with walking and even causing serious falls, are an advanced symptom of toenail fungus. For patients who are already affected by diseases that cause problems with the nerves in the legs, this can make things even worse.
There are four main types of onychomycosis:
- Distal subungual onychomycosis – This is the most common form of onychomycosis and is caused by a dermatophyte called Trichophyton rubrum. What happens is the dermatophyte penetrates the nail plate and buries itself in the nail bed. The term ‘subungual’ refers to underneath the nail. The infection manifests as a whitish-yellow growth under and on the nail towards the tip (the part you trim) This then works its way down toward the cuticule and underneath to the nail bed. The nail becomes thick, pitted, ridged and can start to crumble.
- Proximal subungual onychomycosis – starts at the cuticle end of the nail instead of at the tip. It then works its way up the nail and under the nail as the nail grows out. This form of nail fungus infection occurs more regularly in people who have issues with immune deficiency. Proximal subungual onychomycosis is caused by Trichophyton ruburm, just as distal subungual onychomycosis is, but it is also caused by other fungi and molds.
- White superficial onychomycosis – This is probably the least commonly occurring form of onychomycosis, happening in only 1 of 10 cases on average. This fungus develops on the top of the nail or in its topmost layers. As the name ‘white superficial’ would imply, this is a lesion that forms at the top of the nail and is white in color. Gradually, the fungus will take over the entire nail if left unchecked. Unlike most other forms of onychomycosis, white superficial onychomycosis is caused by Trichophyton mentagrophytes, a different dermatophyte.
- Candida onychomycosis – This final form of onychomycosis starts out its life as chronic mucocutaneous candidas, or reoccurring mucous level or low level yeast infection. This tends to affect the skin surrounding the nail, specifically in the proximal and lateral nail folds. Usually multiple nails are affected by Candida onychomycosis and the nails can be fully destroyed by this more serious form of fungal infection.
References
Hainer BL. Dermatophyte infections. Am Fam Physician 2003;67:101-108.
Jaffe R. Onychomycosis: recognition, diagnosis, and management. Arch Fam Med 1998;7:587-592.
Kaur R, Kashyap B, Bhalla P. Onychomycosis–epidemiology, diagnosis and management. Indian J Med Microbiol 2008;26:108-116.
Onychorrhexis – Brittle Nail Disease
Onychorrhexis – Brittle Nail Disease
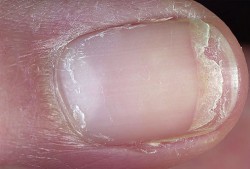 What is it? – When fingernails and toenails break easily because they are weak.
What is it? – When fingernails and toenails break easily because they are weak.- Why is it? – As keratin develops with protein as a component, the nail grows according to the appropriate thickness determined by the body. Your nail thickness is pretty much set at birth. Some people are born with very thin and/or fragile nails
- What causes it? – Humidity at the base of the nail is a common cause. For instance, soaking your hands (or person) in water for a long period of time (taking a bath or doing dishes) on a regular basis. Some people have a hereditary condition of weak nails. As they grow older, their nails become weaker and more prone to breakage. Some diseases and circumstances that might cause a fragile nail are:
- Hypothyroidism or low thyroid levels
- Reynaud’s syndrome
- Skin diseases, such as psoriasis
- Lack of proper nourishment
Signs of this affliction
- Flaking at the base of the nail
- The nails breaking and/or falling off
Basic Treatment
People with brittle nails should not spend a lot of time with their hands in the water. They should dry their hands thoroughly after getting them wet and they should use a mild soap when washing.
Immediately after washing and drying their hands, sufferers of onychorrhexis should apply a moisturizer to the afflicted limb. Two recommended kinds of moisturizer are:
- Standard “beauty” moisturizers, which work to soften the skin. These will provide instant relief and will assist people with this affliction greatly.
- Healing moisturizers, which both soften and infuse the skin with herbal or medicinal remedies as well as acting as a barrier between the water and the nail
Some good preventative measures are as follows:
- Wearing protective covering on hands or feet when immersing them in water
- Not participating in activities that involve being submerged in water, such as swimming.
- Protecting the hands from irritating chemicals
- Supplementing the diet with vitamins and minerals to help the nails become stronger.
- Identifying nutritional deficits that may be causing the nail breakdown and working to increase those areas
Side Effects
The only potential negative side effect of the above treatment is an allergic reaction to a moisturizer. Stay alert for irritation of the skin to indicate that there is sensitivity.